
|
African Journal of Reproductive Health
Women's Health and Action Research Centre
ISSN: 1118-4841
Vol. 7, Num. 2, 2003, pp. 109-111
|
Untitled Document
African Journal of Reproductive Health, Vol. 7, No. 2, Aug, 2003 pp. 109-111
Letter to the Editor
Routine Screening for
HIV Infection in Pregnant Women: A Highly Justified Component of Antenatal
Care in Developing Countries
LI Chukwuali*
Code Number: rh03029
I wish to
comment on an article titled "Routine Screening for HIV Infection in Booked
Antenatal Women: How Justified in Developing Countries?" This
article appeared on pages 7-9 of the African Journal of Reproductive Health, Volume
5, Number 2, August 2001.
The human immunodeficiency
virus and the acquired immune deficiency syndrome (HIV/AIDS) pandemic is
an undisputable reality of our time. With a worldwide prevalence of 36.1
million and an estimated 5.3 million new infections in the year 2000 alone1, the
magnitude of the HIV/AIDS pandemic can be better appreciated. The fact that
an estimated 71.7% of the new infections in the year 2000 occurred in sub-Saharan
Africa alone suggests that the HIV/AIDS pandemic could be described as a
sub-Saharan African problem.
In keeping with the increasing
trend of HIV infection worldwide, the prevalence of HIV seropositivity among
the antenatal population in Nigeria has increased from 4.5% in 1996 to 5.4%
in 19992 and to 8.3% in 2001.3
In view of the recognised
benefits of prior knowledge of a positive HIV status to the pregnant woman,
her unborn baby, the health staff and the society at large, routine testing
for HIV has been recommended4,5 and adopted in most hospitals
in the developed countries. For the same reasons, it has similarly been recommended6 and
adopted in many hospitals in developing countries.
The view expressed by the
authors - that routine HIV screening for booked antenatal patients
in developing countries is unjustified7 - seems
to shift significantly from contemporary progressive thinking. In this era
when efforts should be geared towards standardising medical practice across
the globe, it is unacceptable to suggest a lower standard of care for HIV
positive pregnant women in developing countries. The authors gave the following
reasons to support their view: (1) that most women in developing countries
cannot afford the prohibitive cost of routine HIV screening; and (2) that
there are inadequate structures in place to take care of the HIV positive
pregnant women and their babies. They tried to buttress their position with
the 39% default rate in antenatal HIV screening in their centre. However,
it would appear that such a high default rate was due to inadequate counselling
rather than considerations of cost or the realisation that `nothing more
could be done for them even if it was discovered that they were HIV positive',
as implicated by the authors.
The importance of proper
counselling of patients was demonstrated in one survey8 where
80% of booked antenatal patients supported routine HIV screening but only
44.4% individually accepted it. The low acceptance rate was due to fear of
positive results and lack of knowledge of the availability of measures to
reduce mother-to-child transmission, rather than financial considerations.
This underlies the need for proper education and adequate pre-test counselling
of patients. In another survey of a better counselled obstetric population9,
96% accepted routine HIV screening, giving the following reasons for their
acceptance: prevention of vertical transmission (70%), early treatment if
tested positive (50%), and protection of other patients (40%). Effective
information, education and communication machinery is therefore very important
in promoting the acceptance of routine HIV screening in booked antenatal
patients, apart from the need for the same machinery in promoting general
awareness of HIV infection and its prevention.
To say that routine antenatal
HIV screening in developing countries should be jettisoned because its cost
is prohibitive and unaffordable is akin to saying that the cost of antenatal
HIV screening outweighs other costs of antenatal care and childbirth. Women
in developing countries can go to any length to protect the interest of their
babies. If appropriately counselled, most of them will, at least in the interest
of their babies, afford four hundred naira (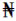 400) (approximately
US$3), which is the average cost of HIV screening in most centres in Nigeria
today. 400) (approximately
US$3), which is the average cost of HIV screening in most centres in Nigeria
today.
If infertile
women and even women of proven fertility who fail to achieve pregnancy within
a self-stipulated time frame can invest a huge amount of money in investigations
and treatment in search of pregnancy, they can spend four hundred naira and
more in the interest of their babies. In most public hospitals, initial antenatal
booking deposit exceeds one thousand naira (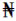 1000.00)
and women who choose to go to such hospitals do not complain and nobody has
succeeded in convincing such hospitals to reduce the fee. Yet hospitals
can readily dispense with such booking deposits without infringing on the
rights of the woman or her unborn child, as would be the case if routine
HIV screening were dispensed with. The pregnant woman and her unborn baby
have a right to the highest standard of care. This human right angle
should always be borne in mind when recommending lower standards of care
for women in developing countries, compared with their counterparts in the
developed countries. 1000.00)
and women who choose to go to such hospitals do not complain and nobody has
succeeded in convincing such hospitals to reduce the fee. Yet hospitals
can readily dispense with such booking deposits without infringing on the
rights of the woman or her unborn child, as would be the case if routine
HIV screening were dispensed with. The pregnant woman and her unborn baby
have a right to the highest standard of care. This human right angle
should always be borne in mind when recommending lower standards of care
for women in developing countries, compared with their counterparts in the
developed countries.
Other components of routine
antenatal investigations, some of them of questionable relevance, cost more
than four hundred naira and women in developing countries have been subjected
to these investigations over the years. Families happily spend money in preparation
for the arrival of their babies. Baby napkins, soap, powder and cream are
common components of such preparation and some of them cost much more than
four hundred naira. Prohibitive cost of HIV screening is, therefore, not
an issue, as mothers spend much more than the cost of HIV screening on other
probably less valuable aspects of antenatal and child care. Appropriate counselling
will orientate the booked patient correctly.
The notion that in the
developing countries the structure for taking care of HIV positive pregnant
women is not in place, and the dismissal of zidovudine and other antiretrovirals
as `not available' and even if available `not affordable' are simply overstatements.
The structure for taking care of HIV positive pregnant women is very much
in place in the developing countries. This structure does not entail drugs
alone but also other multidisciplinary measures to (a) minimise vertical
transmission; (b) ensure that the woman receives optimum care; (c) ensure
adequate counselling on the implications of pregnancy and HIV infection;
(d) minimise the risk of nosocomial infection and other forms of horizontal
transmission; and (e) ensure early involvement of the paediatrician in affected
neonates.
Standard10 and
abbreviated 11 zidovudine regimens as well as the two-dose nevirapine
regimen12 have proven efficacy in reducing vertical transmission.
Granted that these drugs are not readily available and are ordinarily expensive,
the Federal Government of Nigeria recently took delivery of a large consignment
of antiretroviral agents to be dispensed at little or no cost to HIV positive
patients. Besides, there are individuals who can afford these drugs at any
cost and from any source. Such individuals, who may not be aware of their
positive HIV status, could be missed if routine antenatal screening is not
adopted.
Other strategies for minimising
vertical transmission such as avoidance of invasive investigations, elective
caesarean section, vaginal lavage with chlorhexidine, early washing of the
baby and avoidance of breastfeeding are other `structures in place' for taking
care of HIV positive pregnant women and their babies. Although caesarean
section is not a favorite mode of delivery among women in developing countries,
most women accept elective caesarean section if counselled correctly. The
issue of breastfeeding has remained contentious. Some authors13 recommend
breastfeeding to HIV positive women in developing countries because of the
risk of diarrhoeal diseases from bottle feeding. They argue that after all
breastfeeding increases the vertical transmission rate by only 14%.14 However,
other authors15 recommend avoidance of breastfeeding universally.
Despite the controversy, avoidance of breastfeeding is a proven strategy
for minimising vertical transmission, which should be recommended to all
HIV positive women. Educating the women on higher standard of hygiene should
minimise the risk of gastroenteritis from bottle feeding.
We should aim at the highest
standards of care for our patients. In fact, for us in the developing countries,
aiming at a global standard while bearing in mind our gross infrastructural,
socio-cultural and economic impediments avoids complacency and encourages
improvement.
Routine HIV screening for
booked antenatal patients should be adopted universally for the benefit of
the mother, her unborn child, the health community and the society at large.
Proper counselling will improve acceptance rate. The low likelihood of testing
positive and the availability of measures, not necessarily pharmaceutical,
to minimise vertical transmission should from part of pre-test counselling.
Although it could be a devastating experience for a woman to learn of her
positive HIV status in pregnancy, it would be much more devastating for her
to learn that something could have been done to prevent HIV infection in
her baby when the latter is already down with AIDS.
REFERENCES
- Joint United Nations
Programme on HIV/AIDS (UNAIDS) and World Health Organization (WHO) AIDS
Epidemic Update. Geneva: UNAIDS and WHO, December 2000.
- The National AIDS
and STD Control Programme. Department of Primary Health Care and Disease
Control, Federal Ministry of Health. Nigeria, 2000.
- Offiong RA, Bunza
FM and Uya AO. Prevalence of HIV infection among prenatal patients in
Abuja, Nigeria. Trop J Obstet Gynaecol 2001; 18(Supp. 1): 12.
- Mercey D and Nicoll
A. We should routinely offer HIV screening in pregnancy. Br J Obstet Gynaecol 1998;
105: 249-251.
- Carusi D, Learman
LA and Posner SF. Human immunodeficiency virus test refusal in pregnancy:
a challenge to voluntary testing. Obstet Gyneacol 1998; 91: 540-545.
- Cartoux M, Meda
M, Van de Perre P, Nowell ML, Devincenti L and Dabis F. Acceptability of
voluntary HIV testing by pregnant women in developing countries: an international
survey. Ghant International Working Group on Mother-to-Child Transmission
of HIV/AIDS 1998; 12(18): 2489-2493.
- Ibekwe PC and Ikeme
AC. Routine screening for HIV infection in booked antenatal women: how
justified in developing countries? Afr J Reprod Health 2001; 5: 7-9.
- Obi SN, Ezeonu
P and Ezegwui HU. Level of HIV/AIDS awareness and the acceptability of
HIV screening among pregnant women in Abakaliki, Nigeria. Trop J Obstet Gyneacol 2001;
18(Supp. 1): 13.
- Orji EO, Sotiloye
DO, Fawole AO and Huyinbo KI. Attitude of Abeokuta pregnant women to
HIV screening. Trop
J Obstet Gyneacol 2001; 18(Supp 1): 8.
- Connor EM, Sperling
RS, Gelbert R, et al. Reduction of maternal-infant transmission of HIV
type 1 with zidovudine treatment. N Eng J Med 1994; 331: 1173-1180.
- Wade NA, Brikhead
GS, Warren BL, et al. Abbreviated regimens of zidovudine prophylaxis
and perinatal transmission of human immunodeficiency virus. N Eng J Med 1998;
339: 1409- 414.
- Mirochnick M, Fenton
T, Gangnier P, et al. Pharmacokinetics of nevirapine in human immunodeficiency
virus type 1 infected pregnant women and their neonates. J Inf Dis 1998;
178: 368-374.
- Kotler DP. HIV
in pregnancy. Gastroente Clinic of N Am 1998; 27: 269-280.
- Immunodeficiency
virus type 1 transmission through breastfeeding. Lancet 1992;
340: 585-587.
- Olaitan A and Johnson
MA. Human immunodeficiency virus in obstetrics. Prog Obstet Gynaecol 1998;
13: 27-41.
Copyright 2003 - Women's Health and Action Research Centre
|
